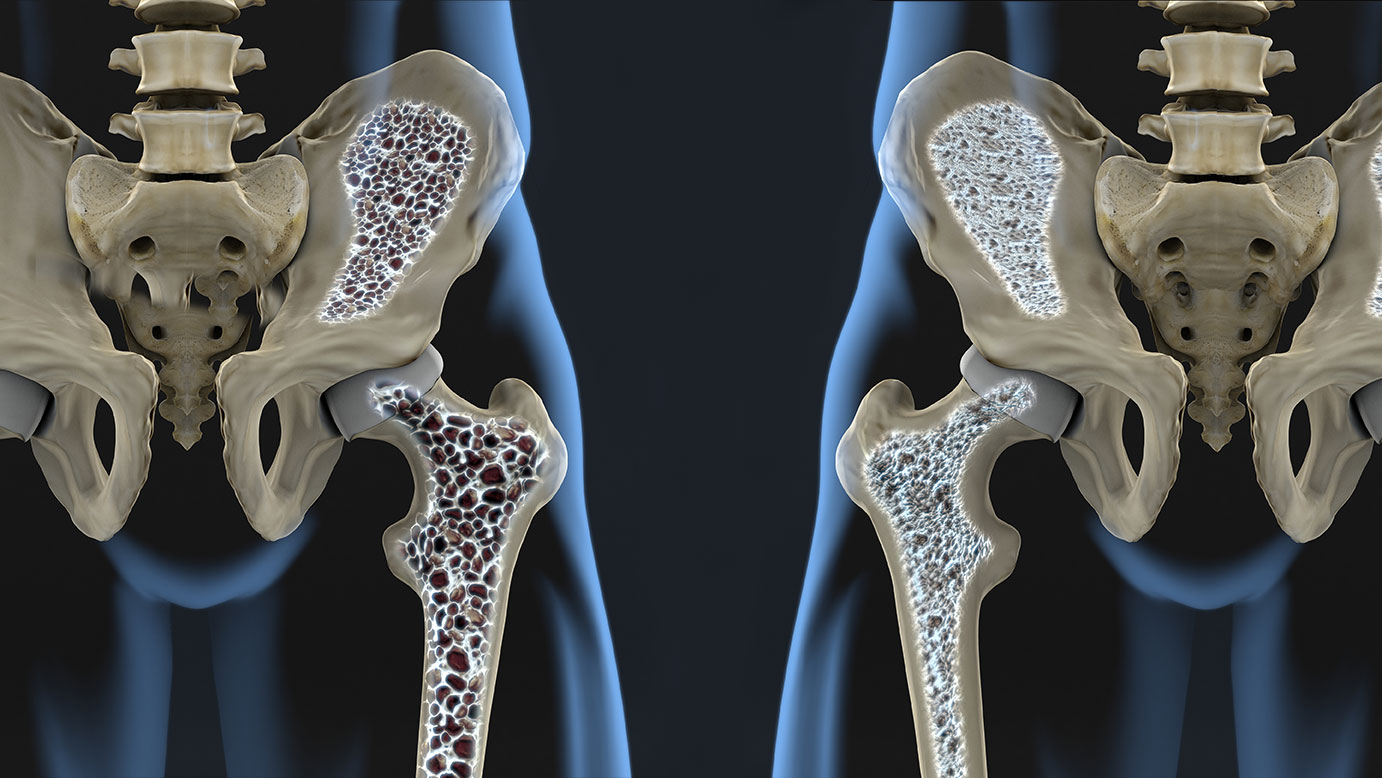
Understanding the Basics of Bone Density
Bone density refers to the amount of mineral matter per square centimeter of bones. It is a critical factor in determining bone strength and overall skeletal health. As we age, our bone density naturally decreases, which can lead to conditions such as osteoporosis—a disease characterized by weak and brittle bones.
Bone density is measured using a dual-energy X-ray absorptiometry (DXA) scan, which provides a T-score indicating how your bone density compares to that of a healthy young adult. A T-score of -1.0 or above is considered normal, while a score between -1.0 and -2.5 indicates osteopenia (low bone mass), and a score of -2.5 or below indicates osteoporosis.
What Causes Bone Deterioration?
Bone deterioration can be attributed to several factors:
- Age: Bone mass peaks in our 20s and gradually declines with age, particularly after menopause in women.
- Hormonal Changes: Particularly in postmenopausal women due to decreased estrogen levels, which accelerates bone loss.
- Nutritional Deficiencies: Lack of calcium, vitamin D, and other essential nutrients can weaken bones.
- Sedentary Lifestyle: Inactivity can lead to weaker bones, as weight-bearing exercises are crucial for maintaining bone strength.
- Medical Conditions: Such as rheumatoid arthritis, hyperthyroidism, and celiac disease can affect bone health.
- Medications: Long-term use of corticosteroids, anticonvulsants, and proton pump inhibitors can contribute to bone loss.
- Genetic Factors: A family history of osteoporosis or low bone density can increase your risk.
The Importance of Early Detection
Early detection of bone density issues is crucial for preventing complications. Regular bone density screenings, especially for women over 50 and men over 60, can help identify potential problems before they become severe. Early intervention can significantly improve outcomes and reduce the risk of fractures.
Doctor-Recommended Therapies for Weak Bones
Doctors often recommend a combination of lifestyle changes, medications, and supplements to treat weak bones. These approaches aim to slow bone loss, strengthen existing bone, and reduce the risk of fractures.
Lifestyle Modifications
- Weight-Bearing Exercises: Activities like walking, jogging, and strength training can stimulate bone growth and improve bone density.
- Balanced Diet: Consuming a diet rich in calcium, vitamin D, protein, and other essential nutrients supports bone health.
- Avoid Smoking and Limit Alcohol: Both smoking and excessive alcohol consumption can weaken bones and increase the risk of fractures.
Medications and Supplements
- Calcium and Vitamin D Supplements: Essential for bone health, especially for individuals with dietary deficiencies or limited sun exposure.
- Bisphosphonates: Medications that slow down bone loss. Examples include Alendronate (Fosamax) and Risedronate (Actonel).
- Parathyroid Hormone (PTH) Therapy: Stimulates bone growth and is typically used for individuals with severe osteoporosis.
- Selective Estrogen Receptor Modulators (SERMs): Mimic estrogen's beneficial effects on bone density without the risks associated with hormone replacement therapy.
- Hormone Replacement Therapy (HRT): Used primarily in postmenopausal women to address estrogen deficiency and reduce bone loss.
Emerging Treatments
Recent advancements in bone density treatments include:
- Romosozumab (Evenity): A monoclonal antibody that promotes new bone formation while reducing bone resorption. It is typically administered monthly for one year.
- Teriparatide (Forteo): A synthetic form of parathyroid hormone that stimulates bone growth. It is often prescribed for individuals with severe osteoporosis.
Advanced Treatments for Osteoporosis
Osteoporosis requires targeted treatments to prevent fractures and maintain quality of life. Advanced treatments are designed for individuals with severe bone density loss or those who have not responded well to initial therapies.
Safest Osteoporosis Treatment Options
-
Bisphosphonates
- Examples include Alendronate (Fosamax) and Risedronate (Actonel).
- These drugs slow down the rate at which bone is broken down, thereby reducing the risk of fractures.
-
Denosumab (Prolia)
- A monoclonal antibody that targets a protein responsible for bone resorption, thereby slowing bone loss.
- Administered via injection every six months, it is particularly effective for postmenopausal women.
-
Teriparatide (Forteo)
- A form of parathyroid hormone that stimulates new bone growth.
- Recommended for those with severe osteoporosis or a high risk of fractures.
-
Romosozumab (Evenity)
- Encourages new bone formation while decreasing bone resorption.
- Administered monthly for a year, it is a promising option for individuals with low bone density.
-
Strontium Ranelate (Protos)
- A medication that stimulates bone formation and reduces bone breakdown.
- Commonly prescribed in Europe and other regions.
Managing Side Effects
While these treatments are effective, they may come with side effects. For example:
- Bisphosphonates can cause gastrointestinal issues, such as heartburn or stomach pain.
- Denosumab may increase the risk of infections or skin reactions.
- Teriparatide is associated with an increased risk of osteosarcoma (a rare type of bone cancer) when used long-term.
It is essential to discuss the potential risks and benefits of each treatment with your healthcare provider to determine the best option for your specific situation.
The Role of Endocrinologist Specialists in Osteoporosis
An endocrinologist specializes in hormonal imbalances and can provide expert care for osteoporosis patients by:
- Tailoring treatment plans based on individual needs, including hormonal factors.
- Monitoring hormone levels that affect bone health, such as estrogen, testosterone, and parathyroid hormone.
- Adjusting medications as necessary to maximize effectiveness and minimize side effects.
Endocrinologists often work in conjunction with other specialists, such as rheumatologists and orthopedic surgeons, to provide comprehensive care for individuals with osteoporosis.
Marginal Osteoporosis: An Overlooked Condition
Marginal osteoporosis, also known as osteopenia, refers to borderline cases where bone density is lower than normal but not low enough to be classified as osteoporosis. While it is less severe than osteoporosis, it is crucial to address this condition early to prevent progression to full-blown osteoporosis.
Risk Factors for Marginal Osteoporosis
- Aging: Bone density naturally decreases with age, making older adults more susceptible.
- Low Calcium Intake: Insufficient dietary calcium can contribute to bone density loss.
- Vitamin D Deficiency: Vitamin D is essential for calcium absorption, and deficiency can lead to weaker bones.
- Family History: A genetic predisposition to low bone density increases the risk.
- Lifestyle Factors: Smoking, excessive alcohol consumption, and a sedentary lifestyle can all contribute to bone density loss.
Preventive Measures
Early intervention is key to managing marginal osteoporosis and preventing its progression. Preventive measures include:
- Calcium-Rich Diet: Consuming foods like dairy products, leafy greens, and fortified cereals can help maintain bone density.
- Vitamin D Supplementation: Especially for individuals with limited sun exposure or dietary deficiency.
- Regular Weight-Bearing Exercises: Activities like walking, jogging, and strength training can strengthen bones and improve balance.
- Avoiding Smoking and Limiting Alcohol: Both smoking and excessive alcohol consumption can weaken bones and increase the risk of fractures.
Can You Rebuild Bone Density?
Rebuilding bone density is possible through a combination of lifestyle changes, dietary adjustments, and medical interventions. While it is easier to maintain bone density than to rebuild it, certain treatments and practices can help improve bone health.
Key Strategies for Rebuilding Bone Density
- Regular Weight-Bearing Exercises: Activities like walking, jogging, and resistance training stimulate bone growth and improve bone density.
- Adequate Calcium and Vitamin D Intake: Ensuring sufficient levels of these nutrients is essential for bone health.
- Avoiding Smoking and Excessive Alcohol Consumption: Both habits can weaken bones and hinder bone density recovery.
- Medications: In some cases, medications like bisphosphonates and teriparatide can help stimulate bone growth and slow bone loss.
The Role of Hormone Replacement Therapy
Hormone replacement therapy (HRT) can be beneficial for postmenopausal women with low bone density. Estrogen plays a critical role in maintaining bone health, and replacing it can help slow bone loss and reduce the risk of fractures. However, HRT is not suitable for everyone and should be carefully discussed with a healthcare provider.
Monitoring Progress
Regular bone density tests can help monitor progress and determine the effectiveness of treatment. Typically, a bone density test is recommended every two years for individuals with marginal osteoporosis or osteoporosis.
Q&A: Common Questions About Bone Health
Q1: What is the best diet for maintaining healthy bones?
A1: A balanced diet rich in calcium, vitamin D, magnesium, and protein is vital for maintaining healthy bones. Foods like dairy products, fish, nuts, seeds, and leafy greens should be included regularly. Additionally, incorporating foods rich in antioxidants, such as berries and dark chocolate, can help protect bones from oxidative stress.
Q2: How often should I have a bone density test?
A2: Women over 65 and men over 70 should have a baseline bone density test. Those with risk factors, such as a family history of osteoporosis or a previous fracture, may need earlier testing as recommended by their healthcare provider. Follow-up tests are typically conducted every two years unless significant changes in bone density are detected.
Q3: Are there natural ways to improve bone health without medication?
A3: Yes! Engaging in regular physical activity, ensuring adequate nutrition, avoiding smoking, limiting alcohol intake, and getting enough sunlight exposure for vitamin D synthesis are effective natural strategies. Additionally, practicing good posture and maintaining a healthy weight can reduce stress on bones and joints.
Q4: Can men develop osteoporosis too?
A4: Yes! While it is more common in women due to hormonal changes after menopause, men are also at risk—particularly those with low testosterone levels or other risk factors like smoking or excessive alcohol use. Men with conditions like prostate cancer or those undergoing treatments that affect hormone levels are also at higher risk.
Q5: How does exercise help in improving bone density?
A5: Exercise, especially weight-bearing and resistance training, helps improve bone density by stimulating bone growth and strengthening existing bone. It also improves balance and coordination, reducing the risk of falls and fractures.
The Role of Specialists in Managing Bone Health
Rheumatologist Specializing in Osteoporosis
A rheumatologist focuses on diseases affecting joints and muscles but also plays a crucial role in managing osteoporosis by:
- Identifying underlying causes related to autoimmune disorders, such as rheumatoid arthritis or lupus.
- Prescribing appropriate medications tailored specifically for each patient’s condition, including bisphosphonates and hormone therapies.
- Monitoring patients for potential side effects of medications and adjusting treatments as needed.
Orthopedic Surgeon
An orthopedic surgeon specializes in injuries and conditions affecting the musculoskeletal system. In cases of severe osteoporosis or fractures, an orthopedic surgeon may be involved in:
- Performing surgical interventions, such as vertebroplasty or kyphoplasty, to stabilize fractured vertebrae.
- Providing recommendations for physical therapy and rehabilitation to improve mobility and reduce the risk of future fractures.
Physical Therapist
A physical therapist can help individuals with osteoporosis improve their strength, balance, and mobility through tailored exercise programs. These programs often include:
- Weight-bearing exercises to strengthen bones.
- Balance training to reduce the risk of falls.
- Flexibility exercises to improve range of motion and overall physical function.
Table 1: Comparison of Common Bone Density Treatments
| Treatment Type | Mechanism | Frequency | Side Effects |
| Bisphosphonates | Slows down bone resorption | Weekly/Monthly | Gastrointestinal issues |
| Denosumab | Inhibits osteoclast formation | Every 6 months | Skin infections |
| Teriparatide | Stimulates new bone growth | Daily | Leg cramps |
| Romosozumab | Promotes new formation & reduces loss | Monthly | Joint pain |
| Strontium Ranelate | Stimulates bone formation | Daily | Headaches, joint pain |
References
- https://academic.oup.com/jbmrplus/advance-article/doi/10.1093/jbmrpl/ziaf087/8132808?searchresult=1
- https://markvanderpump.co.uk/osteoporosis-treatment-and-its-current-challenges/
- https://pmc.ncbi.nlm.nih.gov/articles/PMC12050228/
- https://www.southcarolinablues.com/web/public/brands/medicalpolicy/external-policies/parathyroid-hormone-phosphorus-calcium-and-magnesium-testing/
- https://en.wikipedia.org/wiki/Parathyroid_hormone