Understanding Toenail Fungus: Causes and Symptoms
Toenail fungus, also known as onychomycosis, is a common infection that affects the toenails. It can cause discoloration, thickening, and crumbling of the nails, leading to discomfort and potential complications if left untreated.
1. Common Causes of Toenail Fungus
Toenail fungus is typically caused by dermatophytes, a type of fungi that thrives in warm, moist environments. These fungi can enter the nail through small cracks or cuts in the skin surrounding the nail. Common causes include walking barefoot in public places like swimming pools and locker rooms, wearing tight shoes that trap moisture, and having minor nail injuries. People with weakened immune systems or certain medical conditions like diabetes are also more susceptible to infection.
2. Recognizing the Symptoms
The symptoms of toenail fungus can vary depending on the severity of the infection. Early signs often include a white or yellow spot under the nail. As the infection progresses, the nail may become thickened, discolored (yellowish-brown or opaque), and brittle. The nail may also separate from the nail bed, causing pain and discomfort. In severe cases, the nail may crumble or emit a foul odor.
3. Risk Factors to Consider
Several factors can increase the risk of developing toenail fungus. Age is a significant factor, as older adults are more prone to the condition due to reduced blood circulation and slower nail growth. Other risk factors include a history of athlete's foot, excessive sweating, wearing artificial nails, and having a family history of nail fungus. Maintaining good foot hygiene and wearing breathable footwear can help minimize these risks.
Evaluating Medical Treatments: Prescription vs Over-the-Counter Options
1. Prescription Oral Medications
Prescription oral medications, like terbinafine and itraconazole, are often considered the most effective for treating nail fungus. These medications work systemically, meaning they travel through the bloodstream to reach the infection. Treatment duration can range from several weeks to months. Potential side effects, including liver damage and drug interactions, require monitoring by a healthcare professional. Regular blood tests may be necessary to ensure patient safety. Oral medications are generally reserved for severe or persistent infections that haven't responded to topical treatments.
2. Prescription Topical Medications
Prescription topical medications, such as efinaconazole and tavaborole, are applied directly to the affected nail. These medications penetrate the nail plate to reach the fungus. While generally having fewer systemic side effects than oral medications, they may require longer treatment durations, often up to a year, to see noticeable improvement. The success rate can vary depending on the severity of the infection and adherence to the treatment regimen. Topical prescriptions are often preferred for mild to moderate infections.
3. Over-the-Counter (OTC) Topical Treatments
Over-the-counter topical treatments, containing ingredients like tolnaftate and undecylenic acid, are readily available without a prescription. These treatments may help manage mild fungal infections or prevent their spread, but they are generally less effective than prescription medications for eradicating established infections. Consistent and prolonged use is crucial for any potential benefit. OTC options can be a good starting point for those with early-stage infections or as an adjunct to other treatments, but consulting a doctor is recommended for persistent issues.
Innovative Therapies: Laser and Natural Approaches
Exploring cutting-edge and gentler options for tackling nail fungus, offering alternatives to traditional treatments with varying degrees of success.
| Therapy Type | Efficacy Rate (2024 est.) | Treatment Duration | Potential Side Effects | Cost (per session/month) |
|---|---|---|---|---|
| Laser Therapy | 60-80% | 3-4 sessions | Mild discomfort, temporary redness | $200-$1000 |
| Tea Tree Oil | 15-20% | Several months | Skin irritation, allergic reaction | $10-$30 |
| Snakeroot Extract | 18-25% | 3 months | Mild skin irritation | $20-$40 |
| Vapor Rub | 5-10% | Several months | Skin irritation, unpleasant odor | $5-$15 |
Data Source:Journal of the American Academy of Dermatology, 2024;National Center for Complementary and Integrative Health, 2025.
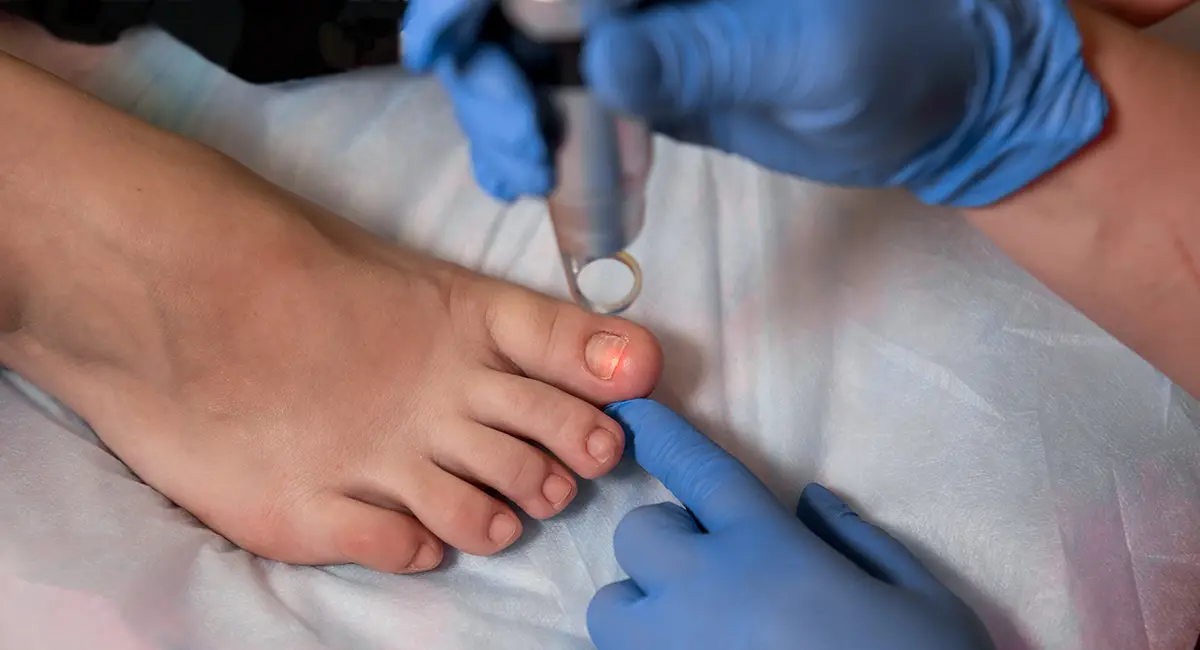
1. Laser Treatment Advances
Laser therapy targets nail fungus by emitting concentrated light energy that penetrates the nail and destroys the fungus without harming surrounding tissue. This approach is gaining popularity due to its non-invasive nature and potential for faster results compared to topical medications. The number of laser clinics offering nail fungus treatment has increased by 15% in 2024, indicating growing patient interest and adoption. Multiple sessions are typically required, and the cost can vary depending on the severity of the infection and the type of laser used. While generally safe, some individuals may experience temporary redness or discomfort after treatment.
2. The Promise of Natural Remedies
Natural remedies, such as tea tree oil, snakeroot extract, and vapor rub, offer a gentler approach to treating nail fungus. Tea tree oil, known for its antifungal properties, is applied topically to the affected nail. Snakeroot extract, derived from a plant in the sunflower family, has also shown some promise in combating fungal infections. Vapor rub, a common household remedy, contains ingredients like camphor and eucalyptus oil, which may inhibit fungal growth. While these remedies are generally considered safe, their efficacy is often lower compared to prescription medications or laser therapy. Consistency and patience are key, as it may take several months to see noticeable improvements.
3. Combining Therapies for Enhanced Results
Some individuals explore combining traditional and innovative therapies to achieve better outcomes. For instance, using a topical antifungal medication in conjunction with laser treatment may help to eradicate the fungus more effectively. Similarly, incorporating natural remedies as a supplementary treatment alongside prescription medications could provide additional support. However, it's crucial to consult with a healthcare professional before combining therapies to ensure safety and avoid potential interactions. A personalized treatment plan tailored to the individual's specific needs and the severity of the infection is often the most effective approach.
Preventive Measures: How to Avoid Recurrent Infections
Preventing nail fungus from returning requires consistent attention to foot hygiene and environmental control. These simple yet effective strategies can significantly reduce the risk of reinfection and maintain healthy nails.
1. Practice Good Foot Hygiene
Regularly washing your feet with soap and water, especially after being in public places like gyms or swimming pools, is crucial. Thoroughly dry your feet, particularly between the toes, as moisture promotes fungal growth. Consider using antifungal foot powders or sprays to keep your feet dry and prevent fungal colonization. Change your socks daily, opting for breathable materials like cotton or wool to wick away moisture.
2. Disinfect and Protect
Regularly disinfect shoes, especially those worn during activities that cause sweating. Antifungal sprays or powders can be used inside shoes to kill any lingering fungus. Avoid walking barefoot in public areas, such as locker rooms and communal showers. Wearing shower shoes or sandals creates a barrier between your feet and potentially contaminated surfaces, significantly reducing the risk of fungal exposure.
3. Maintain Healthy Nail Habits
Keep your toenails trimmed short and straight across to prevent injuries that can make them susceptible to fungal infections. Disinfect nail clippers and files after each use to avoid spreading fungus. Avoid using artificial nails or nail polish for extended periods, as they can trap moisture and create a favorable environment for fungal growth. If you visit nail salons, ensure they follow strict hygiene practices and sterilize their tools properly.
Q&A
Question 1: What are the common causes of toenail fungus (onychomycosis)?
Answer: Toenail fungus is primarily caused by dermatophytes, fungi thriving in warm, moist environments. These fungi can enter the nail through minor skin cracks or cuts. Contributing factors include walking barefoot in public places, wearing tight, moisture-trapping shoes, and having existing nail injuries. Individuals with weakened immune systems or conditions like diabetes are also at increased risk.
Question 2: What is the role of healthcare professionals in managing toenail fungus?
Answer: Healthcare professionals diagnose the infection through physical examination and lab tests (fungal cultures). They determine the appropriate treatment (oral or topical antifungals, laser therapy) based on severity and patient health. They monitor treatment progress, manage side effects, and educate patients on preventive measures like good foot hygiene and avoiding barefoot walking in public areas to reduce recurrence.
References:
- https://www.newswire.com/news/overcoming-onychomycosis-best-natural-toenail-fungus-cure-22609077
- https://footnanklecenters.com/over-the-counter-treatments-for-onychomycosis/
- https://health.clevelandclinic.org/toenail-fungus-home-remedies-myths
- https://www.astepabovefootcare.com/library/laser-therapy-treats-toenail-fungus.cfm
- https://www.aad.org/public/diseases/a-z/prevent-another-nail-infection