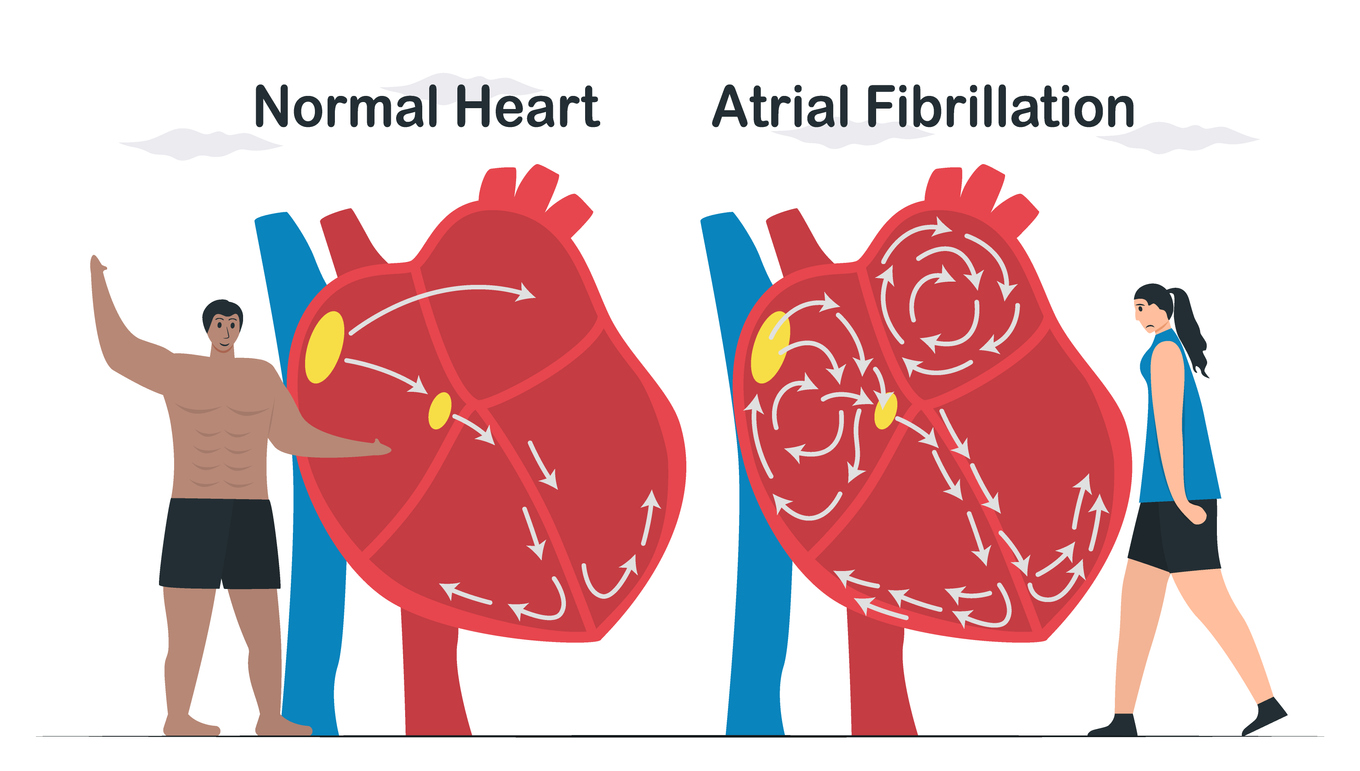
What is Atrial Fibrillation?
Atrial fibrillation is an abnormal heart rhythm where the heart's upper chambers, the atria, beat chaotically and irregularly. Instead of the coordinated contractions that pump blood efficiently to the lower chambers (ventricles) and out to the body, the atria quiver or fibrillate. This irregularity can cause the heart to pump less effectively, increasing the risk of blood clots forming in the atria. If these clots break loose and travel to the brain, they can cause a stroke.
What Happens During Afib?
During an Afib episode, the heart's rhythm is thrown off balance. The atria may beat as fast as 300 to 600 times per minute, while the ventricles usually beat at a slower but still irregular rate. This rapid and irregular beating can lead to several symptoms:
-
Palpitations: Many people with Afib experience a fluttering or pounding sensation in their chest, as if their heart is racing or skipping beats. These palpitations can be quite alarming and may cause anxiety, further exacerbating the symptoms. For example, some patients describe feeling as if their heart is “jumping out of their chest” during an episode.
-
Shortness of Breath: The inefficient pumping of the heart can reduce the amount of oxygenated blood reaching the body, causing breathlessness, especially during physical activity. Even simple tasks like climbing a flight of stairs can become challenging for those with Afib. This is because the heart is unable to supply enough oxygen - rich blood to the muscles, leading to a feeling of being out of breath.
Common Triggers of Atrial Fibrillation
-
Alcohol Consumption: Excessive alcohol intake is a well - known trigger for Afib. Alcohol can irritate the heart's electrical system, leading to abnormal heart rhythms. A study by the American Heart Association found that even moderate alcohol consumption (more than 14 drinks per week for men and more than 7 drinks per week for women) was associated with an increased risk of developing Afib. Alcohol affects the heart in several ways. It can increase blood pressure, which puts additional strain on the heart. It can also disrupt the normal balance of electrolytes in the body, such as potassium and magnesium, which are essential for proper heart function. Moreover, alcohol can cause inflammation in the body, which may contribute to the development of Afib.
-
Caffeine: While caffeine is generally considered safe in moderation, for some individuals, it can act as a trigger. Caffeine stimulates the nervous system, which may affect the heart's electrical activity and potentially lead to an Afib episode. Caffeine works by blocking the action of adenosine, a neurotransmitter that promotes relaxation and sleep. When adenosine is blocked, the body releases other chemicals like adrenaline, which can increase heart rate and blood pressure. For people with a sensitive heart or those already at risk of Afib, this increase in heart rate and electrical activity can be enough to trigger an episode. However, the impact of caffeine can vary from person to person, and some individuals may be able to tolerate higher amounts without any issues.
Afib Triggers and Prevention
Preventing Afib episodes involves identifying and managing the triggers. Here are some strategies:
-
Lifestyle Modifications: Maintaining a healthy lifestyle is crucial. This includes limiting alcohol and caffeine intake, managing stress through techniques like meditation or exercise, and achieving and maintaining a healthy weight. Regular physical activity, such as brisk walking, swimming, or cycling, can improve heart health and reduce the risk of Afib. Exercise helps to strengthen the heart muscle, lower blood pressure, and improve blood circulation. It also helps to reduce stress and anxiety, which are common triggers of Afib. A balanced diet rich in fruits, vegetables, whole grains, and lean proteins can also support heart health. Avoiding processed foods, high - fat foods, and excessive salt intake is important for maintaining a healthy weight and reducing the risk of high blood pressure, which is a risk factor for Afib.
-
Treating Underlying Conditions: Conditions like sleep apnea, high blood pressure, and diabetes should be effectively managed. Treating sleep apnea with continuous positive airway pressure (CPAP) therapy can significantly reduce the risk of Afib in patients with this disorder. High blood pressure puts extra strain on the heart, and controlling it through medications, diet, and exercise is essential. Diabetes can also damage the blood vessels and nerves in the heart, increasing the risk of Afib. Proper management of diabetes, including blood sugar control, can help reduce this risk. Regular check - ups with a doctor are important to monitor and manage these underlying conditions.
Comparing Treatment Options for Afib
|
Treatment Option
|
How It Works
|
Pros
|
Cons
|
|
Medication (Anti - arrhythmic Drugs)
|
Works by blocking or altering the electrical signals in the heart to restore and maintain a normal rhythm. There are different classes of anti - arrhythmic drugs, each with its own mechanism of action. For example, class I drugs block sodium channels, class II drugs are beta - blockers, class III drugs block potassium channels, and class IV drugs block calcium channels.
|
Can be effective in controlling Afib episodes, especially in the short term. Can be taken orally, which is convenient for most patients. Relatively non - invasive compared to other treatment options.
|
May have side effects such as nausea, dizziness, and an increased risk of other arrhythmias. Some anti - arrhythmic drugs can interact with other medications, so careful monitoring is required. Not always effective for long - term management, and some patients may experience recurrence of Afib despite treatment.
|
|
Cardioversion (Electrical or Chemical)
|
Electrical cardioversion uses an electric shock to restore a normal heart rhythm. The patient is sedated, and paddles or patches are placed on the chest to deliver the shock. Chemical cardioversion uses medications, such as ibutilide or procainamide, to convert the abnormal rhythm back to a normal one.
|
Can quickly restore a normal heart rhythm, which is beneficial for patients with severe symptoms or those at high risk of complications. In some cases, it can be a definitive treatment, especially if the Afib is recent and the heart structure is normal.
|
Electrical cardioversion requires sedation, which has its own risks, such as allergic reactions or respiratory problems. There is also a small risk of complications during the procedure, such as skin burns from the paddles or damage to the heart muscle. Chemical cardioversion may have side effects associated with the medications used, such as low blood pressure or abnormal heart rhythms.
|
|
Catheter Ablation
|
Involves inserting a catheter into the heart through a blood vessel, usually in the groin. The catheter is guided to the area of the heart where the abnormal electrical signals are originating. Energy, such as radiofrequency or cryothermal energy, is then delivered through the catheter to destroy the abnormal tissue causing the irregular electrical signals.
|
Can be a long - term solution for some patients, especially those with recurrent Afib that is not well - controlled with medications. It is a minimally invasive procedure compared to open - heart surgery, with a shorter recovery time. Can improve quality of life by reducing symptoms and the risk of complications.
|
A minimally invasive procedure, but still has risks such as bleeding, infection, and damage to the heart tissue or blood vessels. There is also a risk of recurrence of Afib, and some patients may require multiple ablation procedures. The success rate of catheter ablation depends on various factors, such as the type and duration of Afib, the patient's age, and the presence of other heart conditions.
|
Frequently Asked Questions (QA)
Q: Can atrial fibrillation be cured completely?
A: In some cases, Afib can be cured, especially if it is caught early and treated appropriately. Treatments like catheter ablation have been successful in eliminating Afib in many patients. However, for some individuals, Afib may be a chronic condition that requires long - term management with medications and lifestyle changes. The likelihood of a complete cure depends on several factors, such as the type of Afib, the underlying cause, and the patient's overall health. Even if a patient is successfully treated with catheter ablation, there is still a risk of recurrence, and regular follow - up with a doctor is necessary.
Q: Are there any natural remedies for atrial fibrillation?
A: While there are no natural remedies that can replace medical treatment for Afib, certain lifestyle changes can help manage the condition. These include a healthy diet rich in fruits, vegetables, and whole grains, regular exercise, stress management, and limiting alcohol and caffeine intake. Some herbal supplements like omega - 3 fatty acids may have a beneficial effect on heart health, but it's important to consult a doctor before taking any supplements. Omega - 3 fatty acids, found in fish oil, have been shown to reduce inflammation and may help lower the risk of abnormal heart rhythms. However, they should not be used as a substitute for prescribed medications, and they may interact with other medications, so proper medical advice is essential.